Covid-19: How to Track Viral Variants
The emergence of potentially more dangerous SARS-CoV-2 variants highlights the urgency of viral surveillance efforts.
Since the pandemic’s start, virologists knew the virus would change. It could become more dangerous.
And then it did. In December, a SARS-CoV-2 variant sparked a surge of COVID-19 cases in southeast England. Data suggest that this variant is more than 50% more transmissible—and perhaps more deadly. Other variants have since emerged in Brazil and South Africa.
Although every virus accumulates genetic changes over time, the coronavirus mutates more slowly than many other viruses, says Gigi Gronvall, PhD, a senior scholar at the Johns Hopkins Center for Health Security. SARS-CoV-2 showed slow and steady change for much of 2020.
Then the sheer number of cases changed the dynamic. Gronvall notes that every infected patient carries versions of the virus with a variety of mutations, and more patients means more opportunities for the virus to evolve new characteristics, like increased transmissibility.
“It’s a game of chance,” says Andrew Pekosz, PhD, a professor in Molecular Microbiology and Immunology. “If you’ve got a one-in-a-million chance of improving and roll your dice 900,000 times, the likelihood of hitting that one improvement increases vastly.”
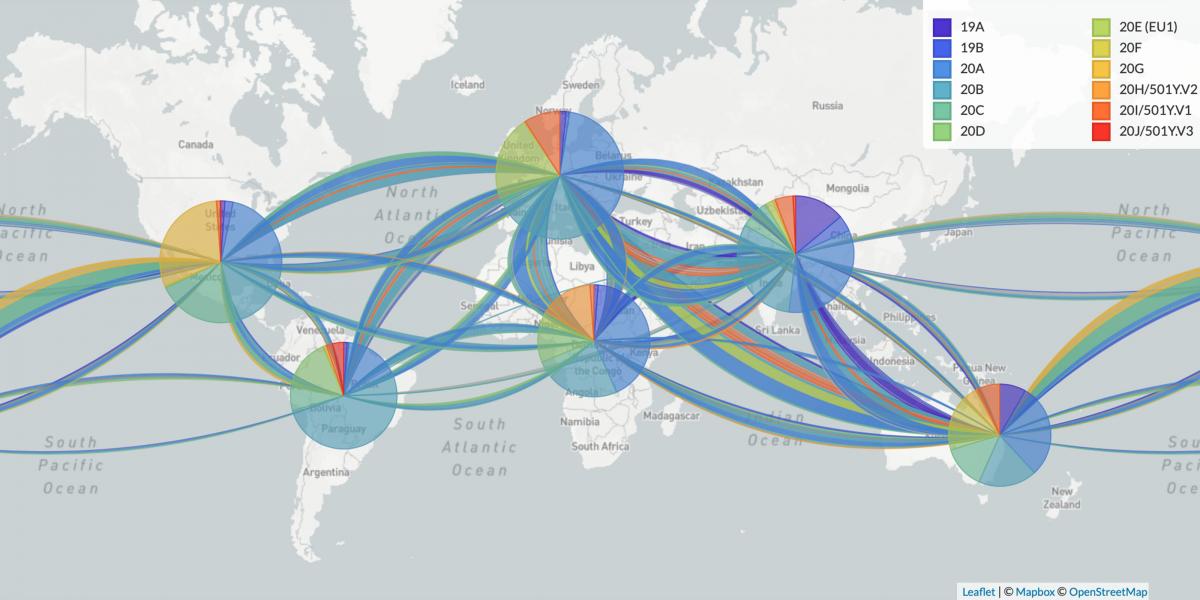
Robust surveillance is essential to find these variants. Pekosz suggests that 25% to 30% of positive tests should be submitted for genomic analysis. These sequences can then be compared against existing genomic data to identify changes that are becoming pervasive.
The UK variant was detected early through such surveillance. The country has been more aggressively sequencing virus genomes from positive tests than the U.S.: 7% versus only 0.32% in the U.S. as of December, according to recent Washington Post analysis. But even the UK falls far short of Pekosz’s recommendations for sequencing SARS-CoV-2 genomes and uploading them to open databases like the GISAID Initiative, Nextstrain, or NCBI’s public archive.
Researchers are especially interested in mutations that affect the spike protein, which the virus uses to infiltrate human cells. This protein is also the primary target of our immune response—including the response induced by current vaccines.
Although all currently approved vaccines appear to hold the UK variant at bay, some data suggest that they may be less effective against those identified in Brazil and South Africa. For example, clinical trials of promising vaccines developed by Novavax and Johnson & Johnson both showed reduced efficacy in areas where these strains are prevalent.
Developing updated vaccines that fend off new variants is a straightforward process. But Gronvall notes that in spite of the variants, the current vaccines are still very effective and could prevent hospitalization and death, so people should get the vaccine when they can.
“We need to do what we can now to reduce transmission generally, as well,” she says.